Understanding Alexander disease


The challenge of diagnosing rare disorders
Nearly 1 in 10 Americans lives with a rare disease—and 50% of them are undiagnosed. Many may see multiple doctors along their diagnostic journey, often receiving misdiagnoses before reaching the right answer. Sometimes, the journey to a correct diagnosis can take years.

For a rare neurological condition like Alexander disease, which can worsen over time, every delay matters. Greater awareness and early recognition can bring clarity sooner and help your doctor guide you toward the best possible care.
What is Alexander disease?
Alexander disease is a rare genetic condition that affects the brain and spinal cord.
It belongs to a group of neurological disorders called leukodystrophies that damage the brain’s white matter (myelin). Myelin acts like insulation around nerve fibers, helping messages travel quickly and smoothly in the brain and body.
Alexander disease is caused by changes (mutations) in a gene called GFAP (glial fibrillary acidic protein). This leads to the buildup of protein clumps—called
Rosenthal fibers—in the brain’s support cells.
![An illustration of healthy myelin on the left and damaged myelin on the right. [78]](/sites/default/files/2026-02/healthy-myelin.png)
HEALTHY MYELIN
![An illustration of healthy myelin on the left and damaged myelin on the right. [78]](/sites/default/files/2026-02/damaged-myelin.png)
DAMAGED MYELIN
Over time, this buildup damages myelin, which can affect how the brain and nervous system work.


The abnormal GFAP gene can sometimes be inherited from a parent, but in most cases of Alexander disease, both parents have normal GFAP genes and the mutation occurs randomly.
Because Alexander disease can look like other neurological disorders, it is sometimes mistaken for conditions such as a brain tumor in children or multiple sclerosis in adults. This means that some people, especially older children and adults, may go years without the right diagnosis.
In infants and young children, the disease is usually diagnosed sooner because their symptoms tend to be more severe and recognizable by others.
What are the common symptoms?
Alexander disease symptoms can first appear in an infant, child, or adult. Symptoms can vary from person to person, often depending on the age when they first appear. If symptoms start in babies or young children, they are usually more severe and progress more rapidly. If symptoms begin later in childhood or adulthood, they may develop more slowly and be less severe.

Infants and children up to 4 years old
- Loss of or delays in reaching milestones (such as sitting, walking, or talking)
- Seizures (sudden episodes of shaking or staring)
- Trouble eating or swallowing foods and liquids
- Frequent vomiting
- Larger-than-usual head size
- Muscle stiffness, spasms, and involuntary contractions
- Difficulty with balance, coordination, or movement

Children older than 4 years of age and adults
- Problems with motor skills (such as balance and walking)
- Difficulty speaking and swallowing
- Frequent vomiting
- Breathing problems
- Heart rate, blood pressure, or digestion problems
- Muscle stiffness, spasms, and involuntary contractions
- Changes in memory or thinking
Remember, these are the most common symptoms by age, but they are not a complete list. Symptoms can vary from person to person and not everyone with Alexander disease will experience all of them.
If you or someone you care for has any of these symptoms,
ask for a referral to a neurologist.


How is Alexander disease diagnosed?
Neurologists—specialists in disorders of the nervous system—use their expertise to diagnose and treat rare conditions like Alexander disease. Through detailed clinical exams, medical imaging such as a brain MRI (magnetic resonance imaging) and genetic testing, neurologists can piece together the clues that lead to an accurate diagnosis and management plan.
Brain MRI
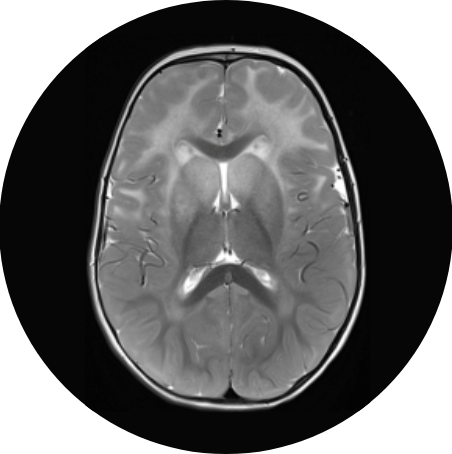
MRI is a painless test that produces detailed pictures of the brain, helping neurologists identify signs of Alexander disease.
Genetic testing

A genetic test is done from a blood, saliva, or cheek swab sample, which is analyzed to look for changes in the GFAP gene that cause the condition.


Getting a confirmed diagnosis as early as possible allows a multidisciplinary care team to create a plan tailored to the patient’s needs—helping manage symptoms sooner and prepare for future treatment options.
Receiving a diagnosis can also enable families to connect with patient advocacy organizations that can provide vital resources, potential financial assistance, and emotional support.
Living with Alexander disease
Currently, there is no treatment or cure for Alexander disease. Care plans focus on coordinated support from different healthcare specialists to manage symptoms and provide comfort. However, researchers are actively studying potential treatments that could directly target the underlying cause of the disease.
Care usually involves a team of specially trained professionals who support patients and their families. This team may include neurologists, physical therapists, speech therapists, nutritionists, and others who can help manage the many symptoms of Alexander disease.

Examples of symptomatic and supportive care
| Seizure management |
|
| Nutrition and feeding |
|
| Movement and muscle support |
|
| Breathing support |
|
| Speech, swallowing, and communication |
|
| Cognitive, emotional, and family support |
|
An earlier diagnosis can help patients by allowing families to access specialized care, manage symptoms sooner, and plan for needed support and resources. For those with advanced disease, palliative care to focus on comfort may be an option.
BiPAP, bilevel positive airway pressure; CPAP, continuous positive airway pressure.

Impact on caregivers
Being a caregiver for someone with Alexander disease can be emotionally and physically demanding. Because the disease is rare and worsens over time, families often face uncertainty and may find it hard to locate healthcare providers who have experience with the condition. Managing daily care, coordinating with specialists, and advocating for your loved one can feel overwhelming.

Access helpful resources for people living with Alexander disease and their caregivers, including links to advocacy organizations and a downloadable guide.